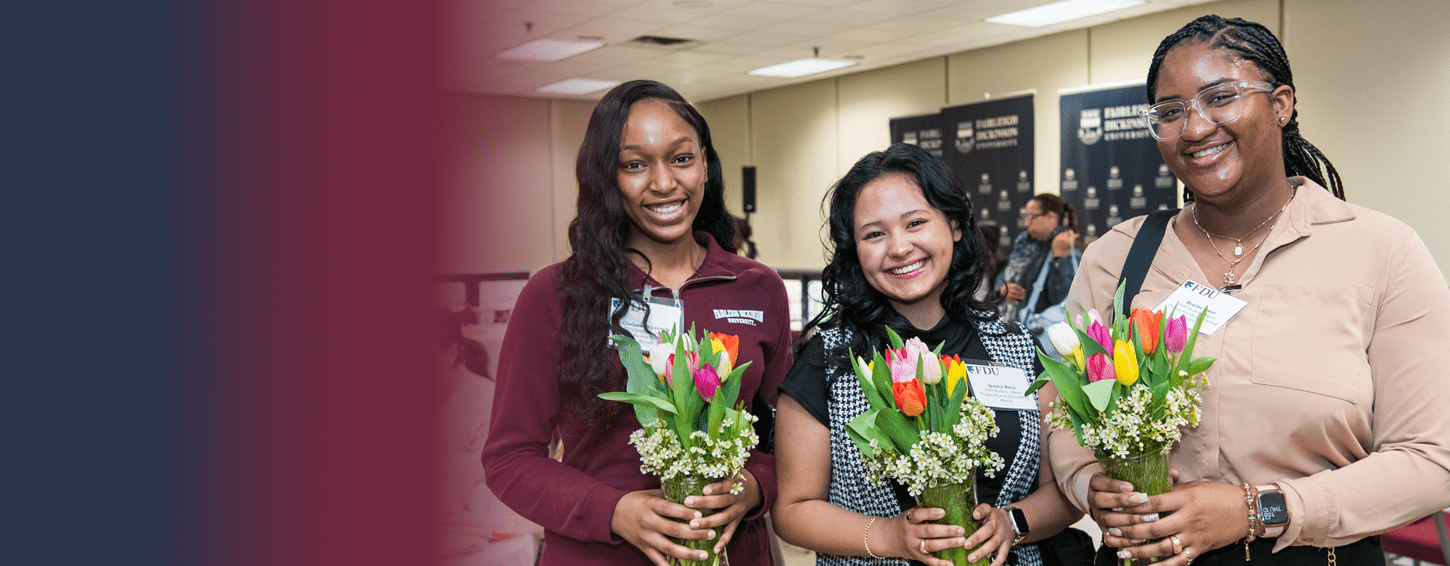Veronica Prisco
Meet FDU Alum Veronica Prisco
On COVID-19 Front Lines

Veronica Prisco is a part of the health care army fighting to save lives and stop the spread of the pandemic.
Veronica Prisco and her husband Jason Prisco, both of whom earned their Doctors of Pharmacy as members of the first graduating class of Fairleigh Dickinson’s School of Pharmacy in 2016, have a new routine when they get home from work.
The couple, who spend all day with the looming threat of potential exposure to COVID-19 and with only limited means of reducing their risk of infection, have had to reconsider almost every part of their day-to-day lives.
“When we get home, we put our clothes in plastic bags and immediately shower,” she says. “No one really knows how long the virus stays on clothing and skin, so, while we are home, we try not to continue that exposure. We have different days off; we are taking turns going to the grocery store; we constantly clean high-touch surfaces.”
“It’s really a change in mentality and being hyper-aware,” she says.
When Prisco accepted a position in the pharmacy of Ridgewood, New Jersey’s Valley Hospital Systems, there was no way to know that the hospital would find itself as a part of the epicenter of New Jersey’s COVID-19 cases. Patients who are positive or presumed positive for the deadly virus now occupy three of the hospital’s four floors.
According to Prisco, hospital staff has had to rethink virtually every process related to patient care that had been in place, including those involving the distribution of medication.
That means that medication reconciliations, the consultations regarding prescribed medicines that hospital pharmacists perform when patients are admitted, are now being performed by telephone instead of in person. The air in many of the rooms in which COVID-19 patients are being treated is being filtered in a way that was once reserved for those rooms in which tuberculosis patients recuperated and chemotherapy and intravenous drugs were being prepared.
Even the way in which the hospital pharmacy is staffed has undergone a sea change. Prisco says that before the current public health crisis, approximately 17 pharmacists worked during the day shift in the main hospital pharmacy. Now, says Prisco, because of new social distancing protocols, only three pharmacists can work in the main pharmacy. Others work off site, in satellite pharmacies in the hospital or in the IV room preparing intravenous medications, the need for which has increased exponentially.
“A lot of the critically-ill patients are intubated,” says Prisco, “so all their medications are IV.”
In addition to working in reconciliation and in the IV room, Prisco has put her studies in healthcare informatics to use, assisting in the upgrade of the Pyxis MedStation, the automated medication dispensing system found at all of the hospital’s nursing units.
“The new version allows us to adjust the meds in critical care and all over the hospital, which provides better support for the nursing staff,” says Prisco. “They can get the meds that they need when they need it as opposed to waiting for pharmacy to deliver them.”
The hospital has instituted other measures to keep staff and patients as safe as possible. Prisco says that, if you’ve been exposed at the hospital, your temperature is monitored daily. And, she says, the hospital recommends that all staff wear surgical masks.
“We have an allotment per employee,” she says. “We got a lot of donations from the community of surgical masks and cloth masks that people are making. The N95 mask is reserved for doctors, nurse and respiratory therapists working directly with patients.”
Prisco says that she is not blind to the risks involved in working at a hospital filled with COVID-19 patients. “I’m probably not alone in this,” she says. “But some of us know we are eventually going to get it. Right now, tests are only approved if you are showing symptoms, even for hospital personnel. I just have to protect myself the best I can and do my job.”